LAPAROSCOPIC AND ROBOTIC HYSTERECTOMY

Director of the Sydney Women’s Endosurgery Centre ( SWEC ), Australia’s leading Centre for the development and training in Advanced Laparoscopic Surgery for women.
This information sheet has been produced for women who want to find out about hysterectomy and in particular the use of Laparoscopic and Robotic Surgery for hysterectomy. Hysterectomy is one of the most common operations performed in Australia and New Zealand and in fact is the second commonest major surgical operation after Caesarean Section being performed in around 33% of women under the age of 60. Medicare data showed that between 2008 and 2010, 43,500 hysterectomies were performed.
WHAT IS A HYSTERECTOMY?
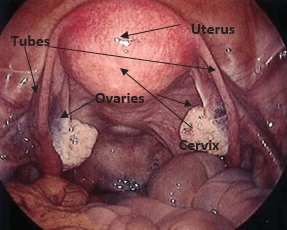
A hysterectomy involves the removal of the womb (uterus) as well as the neck of the uterus (cervix).
In some situations the fallopian tubes may need to be removed (salpingectomy) and the ovaries may need to be removed (oophorectomy). A TOTAL HYSTERECTOMY involves removal of the cervix and the body of the uterus ONLY. It does not mean removal of the ovaries. A Subtotal Hysterectomy leaves the cervix behind. After a hysterectomy there will be no more periods and it is not possible to become pregnant. If a woman is premenopausal and the ovaries are free from disease, they are usually preserved and the patient will not require hormone replacement therapy following surgery. Cyclical symptoms such as sore breasts and mood swings may continue. If the patient is over 5 years past the menopause, if the ovaries are diseased or if there is an indication for reducing the risk of ovarian or breast cancer, the tubes and ovaries may be removed. This is referred to as a Total Hysterectomy and Salpingo-oophorectomy .There is also increasing evidence to suggest that routine removal of the tubes on both sides (bilateral salpingectomy) may be worthwhile in younger patients even if the ovaries are to be reserved as it seems that a proportion of ovarian cancers may begin in the tubes.
WHY DO I NEED A HYSTERECTOMY?
There are a number of reasons why a woman may require a hysterectomy. The commonest of these reasons include troublesome vaginal bleeding and uterine pain not relieved by other treatments. Fibroids may be causing pain, bleeding or pressure effects. Hysterectomy may be performed for symptoms related to endometriosis, as part of an operation for vaginal prolapse and for precancerous changes and cancerous changes in the uterus and/or the cervix.
ARE THERE ALTERNATIVES TO HAVING A HYSTERECTOMY?
- D & C and hysteroscopy (endoscopic examination of the uterine cavity) is a diagnostic procedure and has very little value in the treatment of the above
- Medical Treatment. This includes non-steroidal anti-inflammatory drugs, the oral contraceptive pill, oral progestogens, tranexamic acid (Cyklokapron), Danazol, the progesterone intrauterine device (Mirena) and iron therapy for ana
- Endometrial Ablation. In this surgical procedure the endometrium or lining of the uterus is destroyed down to the level of the muscle coat, essentially removing the entire lining of the uter This procedure has a very high success rate in the first 12 months and a satisfaction rate above 90% with approximately 30-60% of patients having no periods at all. Over the next five years 20-25% of patients will require further intervention, which usually means a hysterectomy.
- Myomectomy, which is the surgical removal of uterine fibroids that can be done at open surgery (particularly for very large fibroids) and at laparoscopic surgery. It’s effectiveness in reducing heavy menstrual bleeding and pelvic pain has been a matter of debate. It is usually reserved for patients who want to preserve their fertility as the operation may have a higher morbidity than hysterectomy with a higher transfusion rate and a higher incidence of postoperative adhesions.
COMMON MYTHS ABOUT HYSTERECTOMY (all of these are not true)
- Hysterectomy causes menopause
- Hysterectomy is my only option
- The Uterus is too big for a Laparoscopic or Robotic Hysterectomy
- Hysterectomy requires 6 weeks for recovery
- Hysterectomy make intercourse worse and stops orgasm
- You cannot have a Laparoscopic or Robotic Hysterectomy if you have had a Caesarean Section
- Subtotal Hysterectomy is better than Total Hysterectomy
- Ovaries should always be removed at the time of Hysterectomy
- A Hysterectomy will cause me to put on weight
HYSTERECTOMY MAY BE PERFORMED IN 4 WAYS:
- The uterus may be removed using an ABDOMINAL HYSTERECTOMY incision, which is either horizontal or vertical. This is performed in most developed countries in up to 60% of
- The uterus may be removed as a VAGINAL HYSTERECTOMY. Here the uterus is removed with the surgeon operating through the vagina. The vagina is sutured from below and there are no scars in the abdomen. (30%) This is usually done for women with significant prolapse of the uterus with no other major pelvic pathology.
- Laparoscopically assisted VAGINAL HYSTERECTOMY where the upper part of the uterus is removed using the keyhole technique and the operation completed using the traditional vaginal approach. This is a form of vaginal hysterectomy only (8-30%)
- TOTAL LAPAROSCOPIC HYSTERECTOMY. The uterus is removed entirely using the standard keyhole technique and the vaginal vault is stitched from abov There is no vaginal surgery with this technique. This was the newest technique. (2-10%)
- ROBOTIC TOTAL LAPAROSCOPIC HYSTERECTOMY. The Uterus is removed using a special 3D Laparoscopic camera and special robotic instruments that have “wrists” that allow a larger range of complex movements than the human hand. The 3D picture and the robotic hands are all controlled by the surgeon sitting at a console in the theatre with the nurse and assistant at the bedsid The surgeon and not the robot performs the surgery. This is the newest form of hysterectomy worldwide and in Australia is limited to very few units outside cancer centres.(<1%)
The very prestigious American Association of Gynaecological Laparoscopists released a policy statement in 2010 after a large review of the world literature stating that ABDOMINAL Hysterectomy in most cases should no longer be performed for benign disease except in exceptional circumstances. A minimally invasive option should always be performed and if surgeons are not trained in these new techniques they should refer to units where Laparoscopic, Robotic or even vaginal options are available.
WHAT IS LAPAROSCOPIC AND ROBOTIC HYSTERECTOMY?
These days laparoscopic or keyhole surgery is used to diagnose most gynaecological problems and a large number of surgical conditions. It has been used successfully for 40 years as a diagnostic tool and over the last 20 years has become the major instrument for performing pelvic surgery in women. Laparoscopic surgery uses conventional “straight sticks” instruments with very long shafts allowing a limited amount of movement and requiring great dexterity to do complicated surgery. Robotic Surgery further refines complex surgery by using 3D technology for improved vision and Robotic “wristed ‘ instruments for improved dexterity allowing much greater precision in dissecting very fine anatomical structures like nerves. It is now the GOLD standard worldwide for Radical Prostate Cancer Surgery and is now having a similar impact on Malignant and Benign Gynaecological surgery. The present Laparoscopic surgery can perform all of the present advanced pelvic procedures successfully but Robotic surgery is a sophisticated form of this and is the future of surgery which will be performed through a single robotic port and the umbilicus in the next few years.
Laparoscopic hysterectomy was first performed in l989 in the USA and was first performed by Dr Cario in 1991 and is now very commonly performed by a number of surgeons throughout Australia. The Robot was introduced into Australia few years ago for urology and only more recently for Gynaecology. It is only available in a very small number of units and only covered by 30% of funds at present. This will all change dramatically in the next few years as its popularity spreads like wildfire as it has done in the USA. You need to contact your funds to enquire if you are covered.
ARE THERE ADVANTAGES TO LAPAROSCOPIC AND ROBOTIC SURGERY?
Laparoscopic surgery is a less traumatic way of removing the uterus and is associated with a dramatic decrease in pain, minimal scarring, less blood loss, faster recovery and a quicker return to normal activities and work. Early indications show that the Robotic Hysterectomy may even be less painful and associated with an even quicker return to normal activities because the robotic instruments movements are controlled by a computer and pivot on the abdominal wall and muscles rather than mechanically distort the muscles with human movement of the laparoscopic instruments.
IS THIS PROCEDURE SAFE?
All types of surgery carry a risk. This risk includes the risk of general anaesthesia and the risk related to the procedure. It appears that laparoscopic hysterectomy has exactly the same major complication rate as abdominal or vaginal surgery. Laparoscopic and robotic surgery has a significant decrease in the minor complication rate because there are less incisions and the recovery time is decreased. Major complications include damage to the bladder, bowel, ureters, major blood vessels, haemorrhage, infection or blood clots. The total rate of these major complications appears to be less than 5-10 per 1000 regardless of whether abdominal, vaginal laparoscopic or a robotic approach is taken. My unit here at THE SYDNEY WOMENS ENDOSURGERY CENTRE (SWEC) have published the complication rates of over l0,000 major laparoscopic cases performed over the last l0 years in peer reviewed journals and the rate of major complications is consistently less than l% Occasionally during an operation the surgeon may discover an additional problem which complicates the procedure. In this situation he may need to convert the operation to an “open incision” laparotomy. This happens in less than l 250 cases.
POSTOPERATIVE CARE.
HOW LONG WILL IT TAKE ME TO RECOVER FROM THE SURGERY?
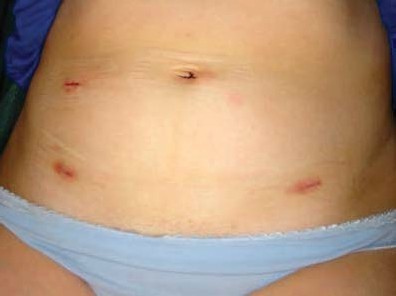
The external incisions are very minor and heal quickly. This is a major operation and the internal healing process may take considerably longer. In our recent review article we showed that the average time in hospital was a little over 2 days with return to normal home activities in around 9 days and return to full time work in around 15 days. A certain amount of discomfort should be expected in the first few days following the operation. During surgery carbon dioxide is used to inflate the abdomen and this may give rise to a dull ache, abdominal bloating and some shoulder tip pain. This discomfort usually passes in 24-48 hours. There may be mild discomfort over the incision sites. Generally speaking, the patient may begin a normal diet almost immediately after surgery and should ambulate very quickly within the first 24 hours. The patient can start driving again 24 hours after discharge from hospital. It is normal to have light spotting or discharge for up to 4-6 weeks after surgery. In the 2nd week after surgery the patient may develop and increasing vaginal discharge or even bleeding which can represent a small haematoma or infection of the healing suture line at the top of the vagina due to bugs travelling from the anal canal into the vagina. It is usually easily treated with antibiotics. It is also the time when women can become very constipated or even impacted. A high fibre diet is essential and often faecal softeners are required. The patient must not lift over 20Kg, perform high impact exercise or have intercourse for 6-8 weeks after surgery.
You should call your doctor if you develop a fever over 38.5.C., heavy vaginal bleeding or offensive vaginal discharge, difficulty emptying your bladder, significant abdominal pain, bloating, nausea, vomiting or, pain, redness and swelling in one of your legs which may indicate a thrombosis.
WHAT IS THE COST OF THE PROCEDURE ?
This practice charges the fees set by the AMA. The Medicare schedule begun in 1975 does not reflect the difficulty or complexity of ground breaking operations like this and in fact they have not even gone to the trouble of providing an appropriate item number to reflect the relative value for this operation despite the fact that we have been doing them for over 20 years. The present item number for Laparoscopic or Robotic Hysterectomy is only marginally higher than the old fashioned “open” hysterectomy item number. Advanced Laparoscopic and Robotic surgery requires many years to master and is only performed by a small group of surgeons in Australia who are certified to perform these operation in particular.
The Medicare system considers operations like this in a similar fashion to plastic surgery where there is a very poor rebate. They feel that the great cosmetic advantage and early release from hospital as well as early return to work are a luxury that people should pay for. There is therefore a considerable gap to pay despite our attempts to lobby the government for a review.
The exact fees and gaps can be easily obtained from my secretary prior to the operation and from the anaesthetist and hospital in a similar fashion. Obviously the big decrease in hospital bed days and the early return to family and work do offset the gap considerably. Please discuss this with me if you have a problem.