LAPAROSCOPIC PELVIC FLOOR RECONSTRUCTION

Information Sheet for patients having a Laparoscopic Prolapse Operation
Dr Greg Cario
FRCOG FRANZCOG
Director of the Sydney Women’s Endosurgery Centre( SWEC), Australia’s leading Centre for the development and training in Advanced Laparoscopic Surgery for Women and
Director of the St George Urodynamic Centre for Pelvic Floor Disorders
WHAT IS THE PELVIC FLOOR?
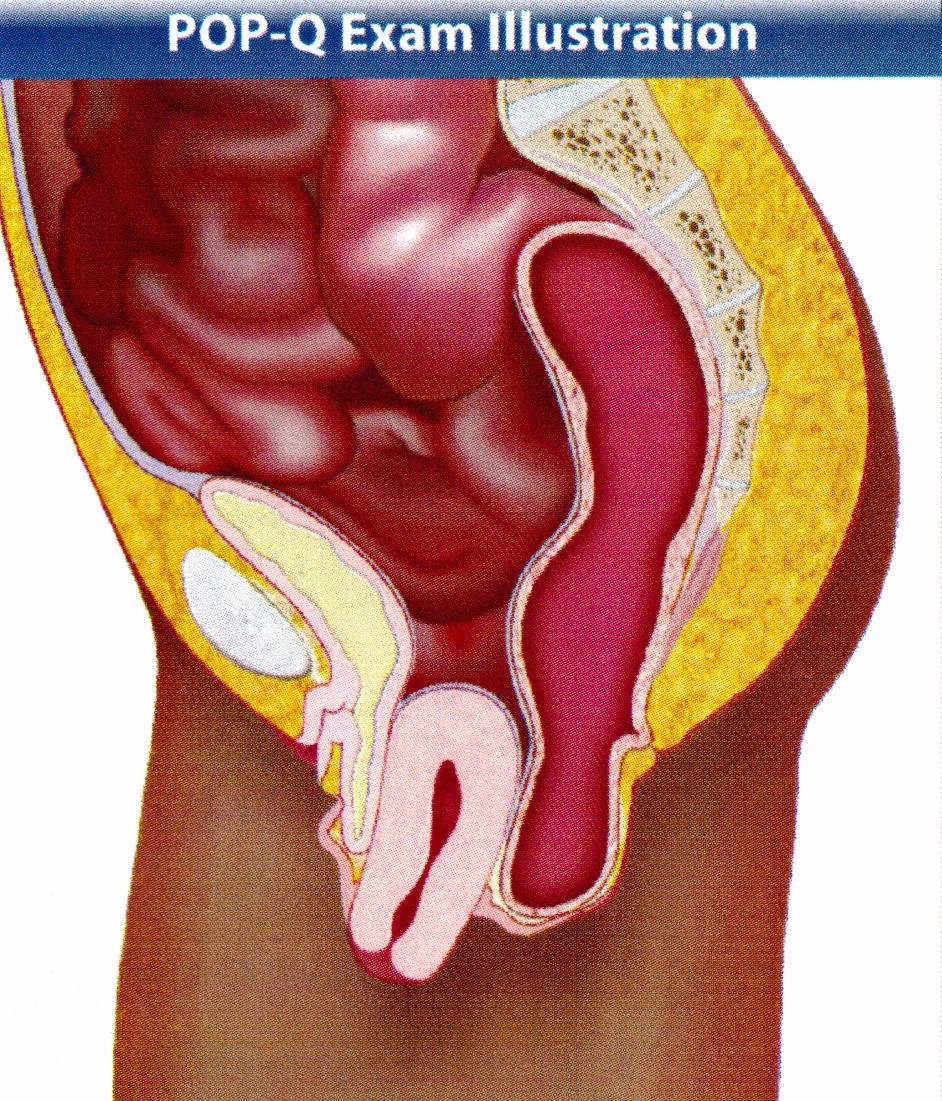
The female pelvic floor is composed of voluntary muscles, fascia and ligaments. These structures have a supportive component and a functional component. They support the bladder, vagina and uterus and the rectosigmoid and are involved in bladder storage, voiding and continence. They are also involved in providing support for the vaginal wall and the cervix and uterus, and also with sexual function. They have a major role in defecation and continence of faeces. Abnormalities of the pelvic floor manifest themselves as urinary incontinence, uterovaginal prolapse, sexual dysfunction and obstructed defecation and faecal incontinence.
WHAT IS PROLAPSE?
About 50% of women will complain of symptoms of vaginal prolapse and 10-20% will undergo surgery with approximately 33% requiring multiple procedures. Urinary incontinence has been dealt with in the information brochure on laparoscopic treatment of urinary incontinence. Genital prolapse involves a weakness at the pelvic floor support mechanisms allowing the organs to herniate through the opening in the pelvic floor muscles .These are divided into compartments. In the anterior compartment we can have simple prolapse of the urethra referred to as a urethrocoele, or the bladder, referred to as a cystocoele. This is often but not always associated with urinary incontinence.
In the middle compartment we can have prolapse of the cervix with the uterus or if a hysterectomy has been performed, prolapse of the top of the vagina referred to as the vaginal vault prolapse. In the posterior compartment we can have a true hernia of the peritoneal body cavity which may involve small bowel which usually affects the upper third of the back wall of the vagina. This is called an enterocoele. When there is prolapse of the rectum, this is called a rectocele. The skin between the vagina and the anus (perineum) may also be deficient and need repair.
WHAT IS LAPAROSCOPIC PROLAPSE SURGERY?
The traditional approach to the repair of prolapse and incontinence has involved a predominantly vaginal approach. This approach is approximately 150 years old. These procedures were refined 100 years ago and 50 years ago the first abdominal procedures were reported which appeared to show a quite marked improvement in the success rate compared to the time honoured vaginal approach. The problem with the abdominal approach was the associated morbidity of open surgery, the large unsightly scar and the longer postoperative recovery phase. As the new techniques for abdominal surgery were evolving, so were the techniques for laparoscopic or keyhole surgery. The first laparoscopic incontinence operation was performed in l991 and since then the evolution of pelvic floor surgery has accelerated dramatically. It became very clear that with the magnification offered by the laparoscope, pelvic floor anatomy could be extremely well visualised and the defects that were causing each of the various types of prolapse could be accurately identified and repaired. Most of these defects were completely invisible using the vaginal approach.
Because of laparoscopic surgery we have developed for the first time, a holistic approach to the pelvic floor. Pelvic floor dysfunction may present as uterovaginal prolapse, urinary or faecal incontinence, voiding and defecation disorders and sexual problems. Each patient who presents with any of these symptoms needs to be assessed in terms of a site-specific anterior compartment defect, middle compartment defect and posterior compartment defect. Surgery needs to be directed towards the site-specific repair of these defects restoring their normal function using the laparoscopic approach which reproduces the various abdominal approaches that have been used for many years and evolving some completely new techniques that would not be possible using the traditional approach.
WHAT ARE THE ADVANTAGES OF LAPAROSCOPIC PROLAPSE SURGERY?
This surgery we believe is more anatomical and capable of restoring normal function without significantly distorting and fibrosing or scarring the vagina in particular which can occur with traditional vaginal surgery. Using these new techniques, the bladder neck can be anchored in a retropubic intra abdominal position. The bladder base can be reattached to the pelvic sidewall. The cervical ring of fascial tissue and ligaments can be reconstituted both with the uterus in position and after hysterectomy. The fascial supports, which act like a fibreglass mesh, keep the anterior and posterior vaginal walls intact. These can be reproduced and anchored to the ligaments around the cervix above, the perineum below and the pelvic floor muscles laterally to try and restore normal anatomy.
In many instances this native tissue “fibreglass mesh” is made up of very poor connective tissue or collagen and will breakdown with time making the likelihood of failure and further surgery more likely. In these instances your surgeon may decide at the time of surgery or in advance in patients with recurrent prolapse to use the new polypropylene mesh or a collagen biological mesh. The SWEC surgeons and Dr Cario in particular have helped introduce this exciting new advance into pelvic floor surgery and he may discuss this with you. It should make the surgery quicker and more reliable with less chance of failure merely replacing the old worn out tissue with a stronger and permanent replacement. There is a risk of infection or rejection of this mesh as with all meshes used in the body, but these new meshes appear to have reduced these complications dramatically especially when the mesh is introduced abdominally or laparoscopically. It is clear however that the extra minor risks of mesh have to be balanced against the dramatically improved success rates. Usually the benefits outweigh the risks substantially
WHAT TYPES OF LAPAROSCOPIC PROLAPSE SURGERY CAN BE PERFORMED?
1 Laparoscopic Anterior Paravaginal or bladder repair to fix anterior prolapse
2 Laparoscopic Colposuspension (also for incontinence) to fix anterior prolapse
3 Laparoscopic Posterior Paravaginal or enterocoele and rectocoele repair to fix posterior prolapse
4 Laparoscopic Uterine suspension to fix middle compartment prolapse to lift the cervix
5 Laparoscopic Hysterectomy to fix middle compartment cervical prolapse
6 Laparoscopic Mesh Sacocolpopexy with or without hysterectomy to fix prolapse in every compartment.
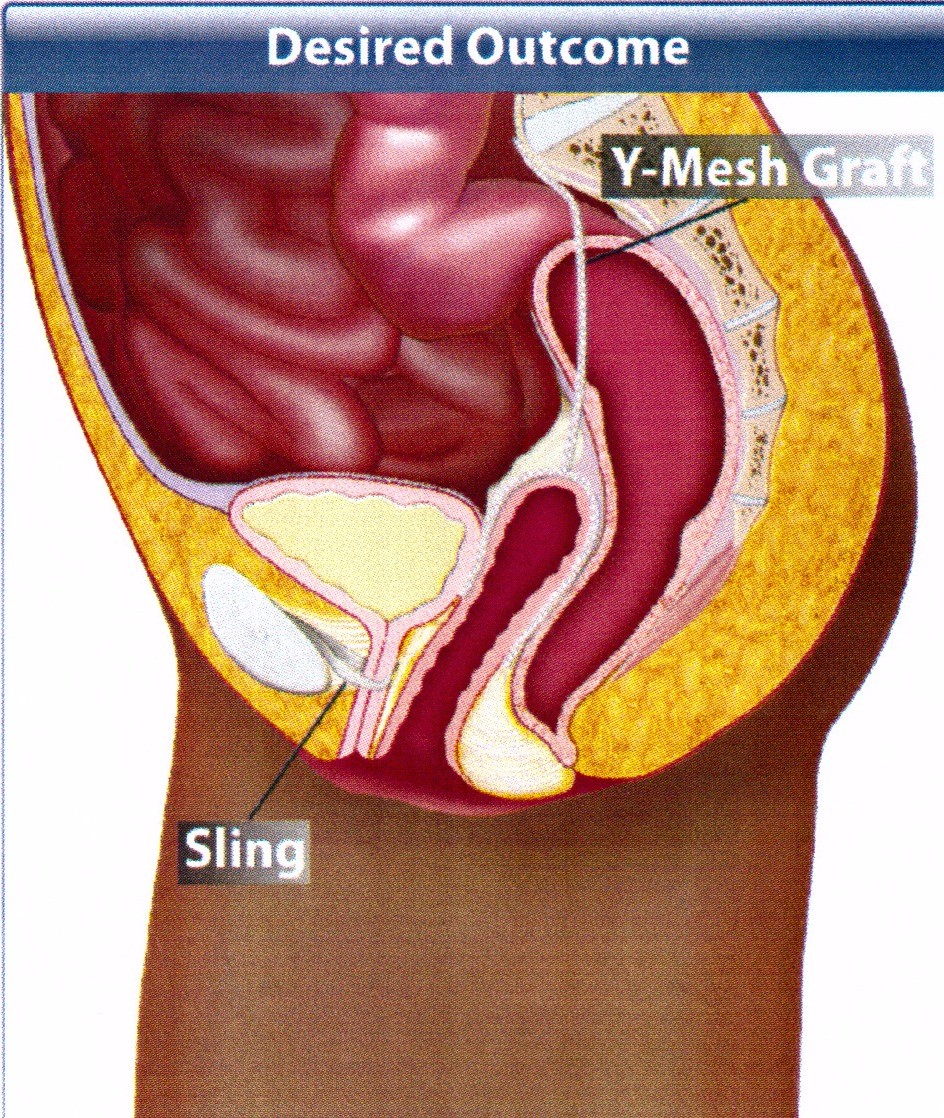
LAPAROSCOPIC MESH SACROCOLPOPEXY THE GOLD STANDARD
This type of severe prolapse involves prolapse of all 3 compartments of the pelvic floor or global prolapse. It is usually driven by prolapse of the cervix and uterus which in turn drags the bladder and bowel down with it. This implies that there is really no reliable support tissue to stitch or reattach and so mesh must be used to provide a durable long term functional result.
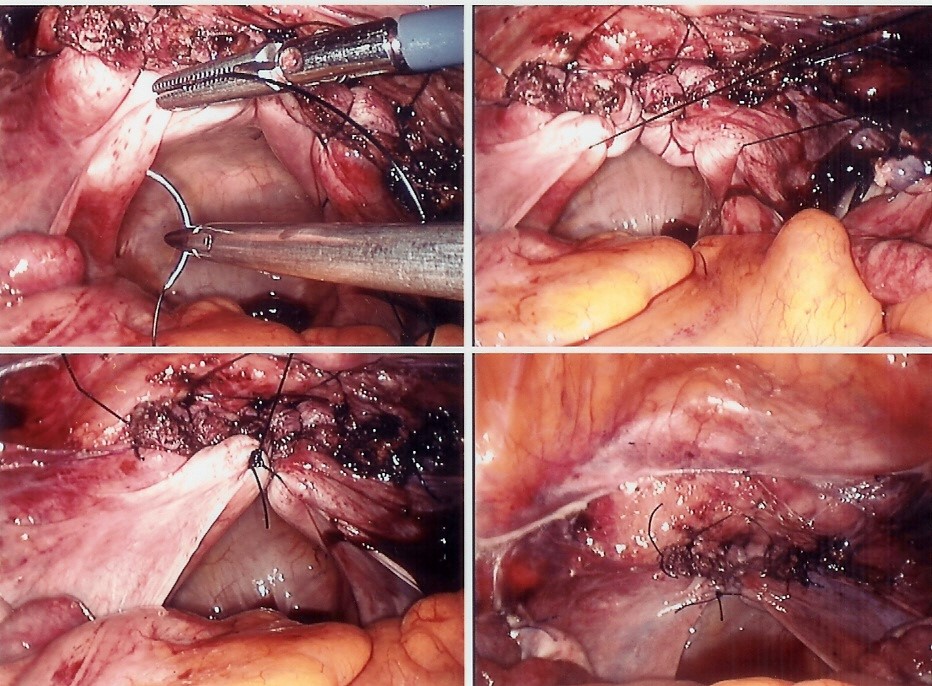
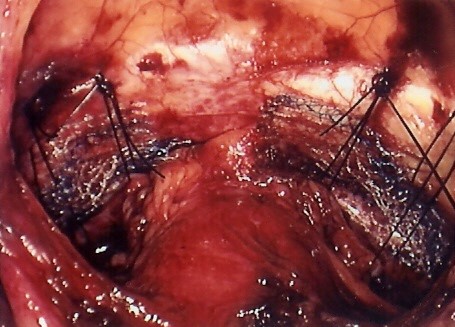
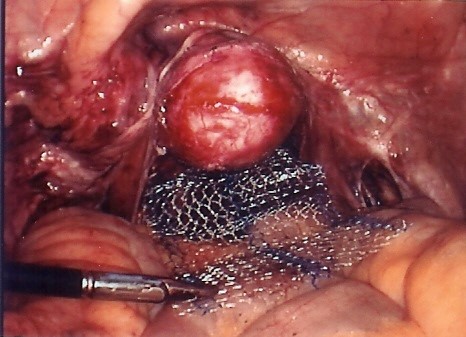
Two mesh grafts are attached in a “Y” shape to the back and front of the vagina and attached high up on the sacrum to elevate the bladder, top of the vagina and bowel back to their normal positions. It has been the Gold Standard for major prolapse for 40 years but was previously done through a big laparotomy cut like the old fashioned hysterectomy and Caesarean Section cut and was a too invasive and painful and patients looked for a more minimally invasive option. The Laparoscope and more recently the Robot and advances in suturing and mesh have meant this has now become very popular in specialist units as the gold standard. It requires no vaginal surgery or incisions with no distortion or scarring of the vagina and restores vaginal length and function to normal with a very rapid recovery and return to normal activities and work .It is also very successful with a long term success rate of over 90% and a mesh complication rate of 1-2%.
IS THE PROCEDURE SAFE ?
All types of surgery including vaginal surgery carry a risk. This will include the risk of the general anaesthesia and the risk related to the procedure itself. These complications include damage to the urethra, bladder, bowel, ureters, major blood vessels, haemorrhage, infection and blood clots. The total rate of these complications would appear to be less than 1%. When mesh is used there may be extra complications related to the mesh itself which include exposure through the vaginal skin and abnormal scarring causing pelvic pain or pain with intercourse. When the mesh is introduced laparoscopically these rates are 1-2% compared with around 15% when the mesh is put in vaginally. In most cases these complications are minor and easily fixed.
Occasionally during an operation a Surgeon may discover an additional problem which complicates the procedure. In this situation he may need to make a number of decisions which might include converting from a laparoscopic operation to an open operation.
There is also a failure rate associated with any type of reconstructive surgery. With traditional approaches and in particular the vaginal approach without mesh, around 33% of women will require at least one further operation due to a recurrence of symptoms. It is hoped that the new laparoscopic approach will dramatically decrease this failure rate but as yet there are no randomised controlled trials to support this but early reports indicate the failure rate may be reduced to about 10%. An enormous amount of data is being gathered prospectively to be reported over the next 5 years.
Depending on the number of defects in the pelvic floor, the operation may last anything from 60 minutes to 180 minutes. If any of these issues is of great concern to you, you must discuss this with your Surgeon.
In summary laparoscopy has provided us with the ideal access to pelvic floor anatomy and the huge advantages in laparoscopic surgical techniques and instrumentations have allowed us to correct these defects for the first time. We believe that the laparoscope has changed forever the treatment of pelvic floor dysfunction. Your doctor will explain to you the type of prolapse that you have and the procedure that would best be performed to correct this. This will often be a combination of the new laparoscopic pelvic floor reconstruction technique and traditional vaginal approaches, which can still be the best method of correction of some simple defects of the bladder base and the low rectum and perineum. Not all patients are suitable for laparoscopic surgery. Some of these operations are quite lengthy and in the older patient it may not be appropriate to have such a long anaesthetic. A traditional vaginal approach may be quicker and simpler and may be recommended by your doctor. Some patients who have had frequent and complicated abdominal surgery may also be unsuitable for the laparoscopic approach.
POSTOPERATIVE RECOVERY
This has been dealt with and is identical to the postoperative instructions for laparoscopic incontinence surgery and vaginal surgery. Please see the brochures on laparoscopic incontinence surgery and vaginal surgery.